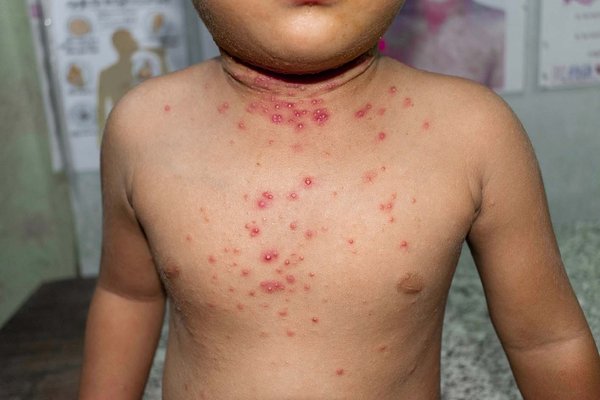
It is quite common to feel overwhelmed when dealing with a skin condition like Molluscum Contagiosum, especially because of how persistent and contagious it can be. Whether you are managing it for yourself or a child, understanding the “why” and “how” of the virus can significantly reduce the anxiety surrounding those little pearly bumps.
Below is a comprehensive clinical guide—a “long case history” style overview—covering everything from the biological causes to the specific aftercare steps needed for recovery.
Comprehensive Clinical Overview: Molluscum Contagiosum
1. Introduction and Etiology (Causes)
Molluscum Contagiosum (MC) is a viral skin infection caused by the Molluscum Contagiosum Virus (MCV), a member of the Poxviridae (poxvirus) family. Unlike many other viruses that can affect internal organs, MCV is strictly “epidermotropic,” meaning it only lives in the outermost layer of the skin (the epidermis) and does not enter the bloodstream.
How it Spreads:
- Direct Skin-to-Skin Contact: The most common route, including normal play among children or sexual contact in adults.
- Autoinoculation: This occurs when an infected person touches or scratches a lesion and then touches another part of their own body, effectively “planting” the virus in a new spot.
- Fomites: The virus can survive on inanimate objects like towels, clothing, toys, gym mats, and razors.
- Environmental Factors: Warm, humid climates and crowded living conditions can increase the rate of transmission.
2. Clinical Presentation (Symptoms)
The hallmark of MC is the appearance of small, firm, raised papules. They typically follow a predictable pattern:
- Appearance: Small, dome-shaped, and “umbilicated” (they have a tiny dent or dimple in the center). They are often pearly, flesh-colored, or slightly pink.
- Size: Usually $2$ to $5\text{ mm}$ in diameter, though they can grow larger in immunocompromised individuals.
- The “Core”: If squeezed (which is strongly discouraged), they contain a white, waxy, or “cheesy” plug known as the molluscum body.
- Sensation: Generally painless, but they can become very itchy, red, or inflamed as the body’s immune system begins to recognize and fight the virus.
3. Types and Variations
While the virus is largely the same, the clinical “type” often depends on the patient profile:
| Type | Target Group | Typical Location |
| Pediatric MC | Children (most common) | Face, trunk, arms, and legs. |
| Adult (Non-STI) | Athletes, gym-goers | Areas of contact (e.g., arms/torso from wrestling). |
| Adult (STI) | Sexually active adults | Genitals, lower abdomen, and inner thighs. |
| Giant Molluscum | Immunocompromised (HIV+) | Can exceed $10\text{ mm}$ and appear in large clusters. |
4. Classification by Patient Type
| Category | Typical Presentation | Key Concerns |
| Pediatric | Clusters on the trunk, armpits, and behind knees. | Spreading to siblings; school/pool restrictions. |
| Adult (Standard) | Often related to gym environments or shared equipment. | Social stigma; slow healing in shaving areas. |
| Adult (Genital) | Papules on the groin, thighs, or lower abdomen. | Classified as an STI; requires screening for other infections. |
| Immunocompromised | “Giant Molluscum” ($>10\text{ mm}$) or hundreds of lesions. | Secondary bacterial infections; high resistance to treatment. |
4. Common Issues and Complications
While the condition is benign (not cancerous), it presents several “quality of life” issues:
- Secondary Infection: Scratching the bumps can introduce bacteria (like Staph), leading to painful, pus-filled sores that require antibiotics.
- Eczema Molluscatum: People with eczema often find the virus spreads much faster because their skin barrier is already “leaky.”
- Psychosocial Impact: Because the bumps can last for 6 to 18 months (and sometimes years), they can cause significant social anxiety, embarrassment, and isolation for children and adults alike.
- Scarring: While the virus itself doesn’t usually scar, aggressive scratching or “home surgeries” often leave permanent marks.
5. Treatment Options
There is a debate in dermatology: “To treat or not to treat?” Since MC is self-limiting (it goes away on its own), many doctors recommend “watchful waiting.” However, treatment is often sought to prevent spread.
Medical Interventions:
- Cryotherapy: Freezing the bumps with liquid nitrogen.
- Curettage: A doctor uses a small tool to “scrape” the lesion core out.
- Cantharidin (“Beetle Juice”): A blistering agent applied by a professional. It causes a small blister under the bump, lifting it off the skin.
- Topical Irritants: Prescription creams like Tretinoin, Salicylic acid, or Imiquimod are used to irritate the skin and “wake up” the immune system to the virus.
6. Precautions and Prevention
To stop the “Molluscum Cycle,” you must be disciplined:
- Don’t Scratch: This is the #1 way it spreads.
- Cover the Bumps: Use clothing or watertight bandages if the bumps are in exposed areas.
- No Sharing: Do not share towels, razors, or unwashed clothes.
- Bathing Habits: Children with MC should be bathed separately from siblings. Use separate towels for the “infected” areas and the “clean” areas of the body.
7. Aftercare and Long-Term Management
If you have undergone treatment (like freezing or scraping), the aftercare is vital to prevent scarring:
- Keep it Clean: Wash the treated area gently with mild soap and water.
- Antibiotic Ointment: If a blister pops or a bump is removed, apply a thin layer of petroleum jelly or prescribed antibiotic ointment to keep the site moist and protected.
- Sun Protection: New skin after a lesion heals is very sensitive. Use sunscreen to prevent the spot from turning dark (hyperpigmentation).
- Monitor for “New Arrivals”: It is common for new bumps to appear even as old ones heal. This is not a “failure” of treatment; it just means those viruses were already incubating under the skin.
Note: Always consult a healthcare provider before starting any home remedies. What works for a wart might be too aggressive for the sensitive skin affected by Molluscum.

