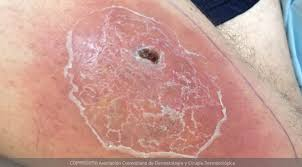
Introduction: Understanding the Depth of Cellulitis
Cellulitis is a common, yet potentially serious, bacterial skin infection that affects the deeper layers of the skin and the underlying soft tissue. Unlike superficial infections that stay on the surface, cellulitis penetrates the dermis and subcutaneous tissues. If left untreated, the bacteria can rapidly spread into the lymph nodes and bloodstream, leading to life-threatening conditions such as sepsis or necrotizing fasciitis.
While cellulitis can appear anywhere on the body, it most frequently affects the lower legs. It typically starts as a small area of pain, swelling, and redness that quickly expands. Because it mimics other skin conditions like dermatitis or deep vein thrombosis (DVT), clinical awareness is crucial for early intervention.
The Causes: How the Barrier Breaks
The primary cause of cellulitis is the entry of bacteria through a break in the skin barrier. Even a microscopic crack can serve as a portal for pathogens.
Common Bacterial Culprits
- Group A Streptococcus: The most frequent cause of rapidly spreading cellulitis.
- Staphylococcus aureus: Including the antibiotic-resistant strain known as MRSA (Methicillin-resistant Staphylococcus aureus).
- Pasteurella multocida: Common in infections resulting from animal bites (cats and dogs).
- Vibrio vulnificus: Often linked to exposure to salt water or brackish water.
Risk Factors and Portals of Entry
- Skin Injuries: Cuts, blisters, burns, or surgical incisions.
- Chronic Skin Conditions: Eczema, athlete’s foot (tinea pedis), or psoriasis that causes the skin to crack.
- Lymphedema: Chronic swelling of the limbs interferes with the immune response in that area.
- Circulatory Issues: Poor blood flow in the legs increases the likelihood of infection.
- Weakened Immune Systems: Conditions like diabetes, HIV/AIDS, or the use of immunosuppressant drugs.
Identifying the Symptoms
Recognizing cellulitis early is the key to preventing hospitalization. Symptoms are generally divided into “localized” (at the site) and “systemic” (affecting the whole body).
Localized Signs
- Expanding Redness: An area of skin that turns red and grows in size over hours.
- Swelling: The skin may appear tight, glossy, or “stretched.”
- Warmth: The infected area feels significantly hotter than the surrounding skin.
- Tenderness and Pain: The site is often very painful to the touch.
- Skin Dimpling: In severe cases, the skin may resemble an orange peel (peau d’orange).
Systemic Signs (Emergency Indicators)
If the infection enters the bloodstream, you may experience:
- Fever and chills.
- Dizziness or lightheadedness.
- Increased heart rate.
- Red streaks radiating from the initial site (lymphangitis).
Types of Cellulitis
Cellulitis is often categorized by the location of the infection or the specific circumstances of its development.
| Type | Description |
| Periorbital Cellulitis | Affects the eyelids and tissues around the eye. Common in children. |
| Orbital Cellulitis | A medical emergency affecting the fat and muscle within the eye socket. |
| Facial Cellulitis | Occurs on the face, often following a sinus or dental infection. |
| Breast Cellulitis | Frequently seen post-surgery or in women with inflammatory breast cancer. |
| Perianal Cellulitis | Infection around the anus, most common in young children. |
Treatment Modalities
The cornerstone of cellulitis treatment is antibiotic therapy. Doctors determine the delivery method based on the severity of the infection.
1. Oral Antibiotics
For mild to moderate cases caught early, a 7-to-14-day course of oral antibiotics (such as Cephalexin or Dicloxacillin) is standard. It is vital to finish the entire prescription even if symptoms improve within 48 hours.
2. Intravenous (IV) Antibiotics
Hospitalization and IV fluids are required if:
- The patient has a high fever.
- The infection is near the eyes.
- Oral antibiotics have failed.
- The patient is immunocompromised.
3. Pain Management
Over-the-counter anti-inflammatories like Ibuprofen can help manage pain and reduce localized swelling.
Aftercare and Long-term Recovery
Recovery doesn’t end when the last pill is swallowed. Proper aftercare prevents recurrence, which is common in chronic cases.
Immediate Post-Infection Care
- Elevation: Keep the affected limb elevated above the heart level to reduce swelling. This uses gravity to help drain excess fluid.
- Rest: Avoid strenuous activity that might irritate the site.
- Wound Care: If there was a physical cut, keep it clean and covered with sterile bandages as instructed by a professional.
Preventing Recurrence
- Moisturize: Use high-quality lotions to prevent skin from cracking or peeling.
- Foot Hygiene: Inspect feet daily for signs of athlete’s foot or small nicks.
- Prompt First Aid: Treat even minor scratches with antiseptic ointment and a bandage immediately.
- Weight Management: Reducing weight can alleviate pressure on the circulatory system in the legs.
Summary Table: Cellulitis Quick Reference
| Category | Key Details |
| Primary Cause | Bacteria (Staph/Strep) entering through skin breaks. |
| Classic Signs | Redness, warmth, swelling, and pain. |
| Urgent Signs | High fever, red streaks, or confusion. |
| Main Treatment | Prescription antibiotics (Oral or IV). |
| Top Prevention | Skin hydration and meticulous wound care. |
A Note on Seeking Help: If you notice a red rash that is spreading rapidly or “tracking” up a limb, do not wait. Early treatment with antibiotics typically clears cellulitis within a few weeks, but delay can lead to permanent lymphatic damage or systemic illness.

