Introduction: Understanding the Silent Struggle
Alopecia Areata (AA) is a complex, unpredictable autoimmune disease characterized by non-scarring hair loss. Unlike typical male-pattern baldness, which is driven by hormones and genetics over decades, AA occurs when the body’s immune system mistakenly attacks its own hair follicles.
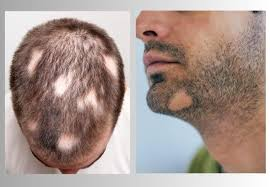
The impact of AA extends far beyond the physical loss of hair. For many, it represents a profound psychological challenge, affecting self-esteem, social interactions, and mental health. While it can occur at any age, it frequently manifests in childhood or young adulthood, often appearing as sudden, smooth, circular patches of hair loss on the scalp.
2. Clinical Symptoms and Manifestations
The onset of Alopecia Areata is often asymptomatic, meaning the individual may not feel anything until they notice a bald spot. However, there are specific clinical signs to watch for:
- Patchy Hair Loss: The hallmark of the condition is the appearance of one or more “coin-sized” patches on the scalp or body.
- Exclamation Point Hairs: These are short hairs that get narrower at the base, found at the edges of expanding patches.
- Nail Abnormalities: In about 10–20% of cases, patients notice “pitting” (tiny dents), redness, or roughness on their fingernails and toenails.
- Sensory Changes: Some patients report a tingling, itching, or burning sensation on the skin shortly before the hair falls out.
- Diffuse Thinning: In rarer cases, hair may thin globally rather than in distinct patches.
3. Etiology: Why Does It Happen? (Causes)
The exact cause of Alopecia Areata remains a subject of intense scientific study, but it is widely accepted to be a polygenic autoimmune condition.
The Autoimmune Mechanism
Under normal conditions, hair follicles are “immune privileged,” meaning they are protected from the body’s immune surveillance. In AA, this privilege breaks down. T-cells (a type of white blood cell) surround the follicle like a “swarm of bees,” causing inflammation that forces the hair into a premature resting phase (telogen).
Genetic Predisposition
While not a strictly “hereditary” disease in the traditional sense, genetics play a massive role. Individuals with a family history of AA or other autoimmune disorders (like Type 1 Diabetes, Rheumatoid Arthritis, or Thyroiditis) are at a higher risk.
Environmental Triggers
While the immune system is the “gun,” environmental factors are often the “trigger.” These may include:
- Severe Stress: Though controversial, many patients link flare-ups to periods of extreme emotional or physical trauma.
- Viral Infections: Certain viruses may confuse the immune system into attacking the follicles.
- Nutritional Deficiencies: Low levels of Vitamin D or Iron may exacerbate the condition, though they are rarely the primary cause.
4. Classifications: The Types of Alopecia Areata
Alopecia Areata is an umbrella term. The condition is categorized based on the extent and pattern of hair loss:
| Type | Description |
| Patchy Alopecia Areata | The most common form; one or more coin-sized bald spots. |
| Alopecia Totalis (AT) | Complete loss of all hair on the scalp. |
| Alopecia Universalis (AU) | The most severe form; loss of all hair on the entire body, including eyebrows, lashes, and pubic hair. |
| Ophiasis Alopecia | A specific pattern where hair loss occurs in a “wave” or band-like shape around the back and sides of the head. |
| Diffuse Alopecia Areata | Sudden thinning across the whole scalp rather than patches; often mistaken for Telogen Effluvium. |
5. Current and Emerging Treatments
There is currently no permanent “cure” for Alopecia Areata, but many treatments can help “turn off” the immune attack and stimulate regrowth.
A. Topical and Localized Treatments
- Corticosteroid Injections: The “gold standard” for patchy AA. A dermatologist injects steroids directly into the bald patches every 4–6 weeks to suppress local inflammation.
- Topical Minoxidil: Often used as a secondary treatment to help speed up regrowth once the inflammation is controlled.
- Anthralin: A synthetic tar-like substance that irritates the skin to “distract” the immune system.
B. Systemic Treatments (Internal)
- Oral Steroids: Used for rapid, widespread loss, though long-term use is limited by side effects like weight gain and bone density loss.
- JAK Inhibitors (The Breakthrough): This is the modern frontier. Drugs like Baricitinib and Ritlecitinib are FDA-approved specifically for severe AA. They work by blocking the cellular signaling pathways (Janus Kinase) that tell the immune system to attack the follicle.
C. Immunotherapy
- DPCP (Diphencyprone): A chemical is applied to the scalp to cause an allergic reaction. This “controlled” allergic contact dermatitis somehow resets the immune response, allowing hair to grow back.
6. The Psychological Impact and Management
Living with AA is often a journey of resilience. Because the hair loss is unpredictable—regrowing in one spot only to fall out in another—it creates a “rollercoaster” of hope and grief.
- Support Groups: Connecting with others through organizations like the National Alopecia Areata Foundation (NAAF) is vital.
- Cosmetic Solutions: Wigs, hairpieces, and eyebrow microblading are excellent tools for reclaiming confidence during active flare-ups.
7. Conclusion
Alopecia Areata is a testament to the complexity of the human immune system. While the condition can be devastating, the medical landscape has changed drastically in the last five years. With the advent of JAK inhibitors and a deeper understanding of autoimmune genetics, the path toward consistent, long-term management is clearer than ever before. If you suspect you have AA, early intervention with a dermatologist is the best step toward recovery.

