Introduction
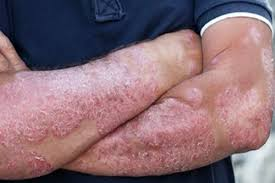
Psoriasis is a chronic, non-contagious autoimmune condition that accelerates the life cycle of skin cells. It causes cells to build up rapidly on the surface of the skin, forming scales and red patches that are often itchy and sometimes painful. Beyond the physical symptoms, it can significantly impact a patient’s quality of life. Understanding that this is a systemic condition—not just a “skin rash”—is the first step toward effective management.
Types of Psoriasis
- Plaque Psoriasis: The most common form, characterized by dry, raised, red skin lesions (plaques) covered with silvery scales.
- Guttate Psoriasis: Primarily affects young adults and children. It is marked by small, drop-shaped scaling lesions on the trunk, arms, or legs.
- Inverse Psoriasis: Occurs in skin folds (armpits, groin, under breasts), appearing as smooth patches of red, inflamed skin.
- Pustular Psoriasis: A rarer form that develops quickly, characterized by white pustules surrounded by red skin.
- Erythrodermic Psoriasis: The least common but most severe type, which can cover the entire body with a red, peeling rash that itches or burns intensely.
Causes and Triggers
While the exact cause remains unknown, it is widely accepted as an immune system issue where infection-fighting cells attack healthy skin cells by mistake.
- Genetics: Family history plays a significant role.
- Triggers: Common triggers include stress, skin injuries (cuts/burns), certain medications (like Lithium), and infections such as strep throat.
- Lifestyle: Smoking and heavy alcohol consumption are known to worsen flare-ups.
Treatment Options
Management focuses on stopping skin cells from growing so quickly and removing scales.
- Topical Treatments: Corticosteroids, Vitamin D analogues, and retinoids are used for mild to moderate cases.
- Phototherapy (Light Therapy): Controlled exposure to natural or artificial ultraviolet (UV) light can reduce symptoms.
- Systemic Medications: For severe cases, oral or injected medicines like Methotrexate or Cyclosporine may be prescribed.
- Biologics: Modern treatments that target specific parts of the immune system to prevent the overproduction of skin cells.
Aftercare and Management
Long-term relief requires consistent lifestyle adjustments:
- Moisturize Daily: Use heavy, ointment-based moisturizers to trap water in the skin.
- Dietary Changes: Incorporate anti-inflammatory foods (Omega-3 fatty acids, leafy greens).
- Stress Management: Yoga, meditation, or therapy can help reduce the frequency of flare-ups.
- Avoid Harsh Products: Use fragrance-free soaps and avoid hot water during showers.
Conclusion
While there is currently no permanent cure for psoriasis, modern dermatology offers a wide array of treatments that can lead to near-total clearance of the skin. By identifying your specific type and triggers, and working closely with a specialist at Grazia Skin Care Clinic, you can manage the condition effectively and lead a comfortable, confident life.https://www.youtube.com/channel/UCQ7voC1nMq0sgVZ2DeDvpCQ

