Introduction
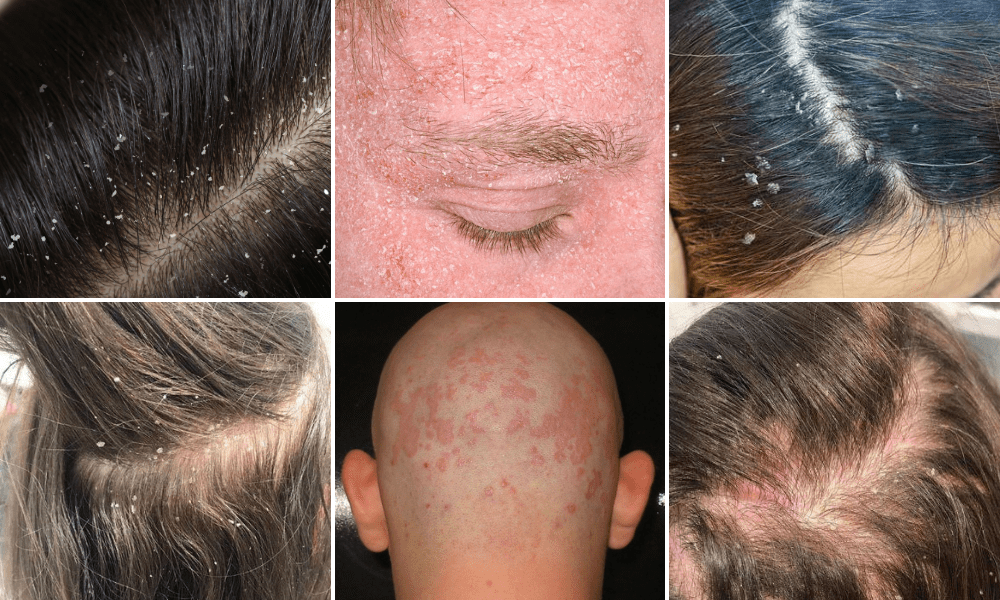
Seborrheic dermatitis is a chronic, inflammatory skin condition characterized by erythematous plaques with oily, yellowish scales. Primarily affecting areas rich in sebaceous glands—such as the scalp, face, and chest—it is a common condition that affects approximately 3% to 5% of the global population.
At Grazia Skin Clinic, we recognize that while seborrhea is not contagious or a sign of poor hygiene, it can significantly impact a patient’s self-esteem and quality of life. This study explores the pathophysiology, clinical manifestations, and modern therapeutic approaches to managing this persistent condition.
Causes and Pathophysiology
The exact etiology of seborrhea remains multifaceted, involving a delicate interplay between host genetics, skin barrier function, and microbial flora.
1. Malassezia Yeast Colonization
The primary biological driver is the proliferation of Malassezia (formerly Pityrosporum), a yeast-like fungus that naturally resides on the skin. In individuals with seborrhea, this yeast breaks down sebum into inflammatory fatty acids, triggering an immune response.
2. Sebaceous Gland Activity
Seborrhea typically emerges during periods of high hormonal activity (infancy and puberty), suggesting that androgen-driven sebum production provides the necessary “fuel” for the condition to thrive.
3. Neurological and Systemic Factors
There is a noted increase in prevalence among patients with neurological disorders (such as Parkinson’s disease) and those with compromised immune systems (HIV/AIDS), indicating a systemic component to skin barrier regulation.
Types of Seborrhea
Seborrhea presents differently depending on the age of the patient and the severity of the inflammation.
- Infantile Seborrheic Dermatitis (“Cradle Cap”): Appears in newborns as thick, crusty, yellow scales on the scalp. It is usually self-limiting and clears by age one.
- Adult Seborrheic Dermatitis: A chronic, relapsing condition that typically begins in late adolescence.
- Sebopsoriasis: An overlap condition where features of both seborrheic dermatitis and psoriasis are present, often requiring more aggressive systemic treatment.
Clinical Symptoms
Patients at Grazia Skin Clinic typically report a combination of the following:
- Skin Lesions: Patches of greasy skin covered with flaky white or yellow scales.
- Pruritus (Itching): While not always present, it can range from mild irritation to intense discomfort.
- Erythema: Redness of the skin, particularly in the nasolabial folds, eyebrows, and behind the ears.
- Blepharitis: Crusty redness on the eyelids.
Treatment Modalities
Because seborrhea is chronic, treatment focuses on management rather than a permanent cure.
Topical Antifungals
The frontline of treatment involves reducing the Malassezia population.
- Ketoconazole 2%: Available in creams and shampoos.
- Ciclopirox: Effective for both its antifungal and anti-inflammatory properties.
Anti-inflammatory Agents
To calm acute flare-ups, low-potency topical corticosteroids or calcineurin inhibitors (like Tacrolimus) are used to reduce redness and swelling.
Keratolytic Agents
Shampoos containing Salicylic Acid, Coal Tar, or Selenium Sulfide help soften and remove thick scales, allowing other medications to penetrate the skin more effectively.
Aftercare and Long-Term Maintenance
Consistency is the key to preventing recurrence. At Grazia Skin Clinic, we recommend:
- Regular Cleansing: Use a pH-balanced cleanser to remove excess oil without stripping the skin barrier.
- Stress Management: Stress is a known trigger for inflammatory “flares.”
- UV Exposure: Moderate, controlled sunlight can sometimes improve symptoms, though sun protection remains essential.
- Scalp Hygiene: Use medicated shampoos 2–3 times a week even during periods of remission.

