1. Introduction: Understanding the Mycological World
Fungi are everywhere—in the air, the soil, on plants, and even naturally on the human skin. While most fungi are harmless, certain species can become “opportunistic pathogens.” A fungal infection, or mycosis, occurs when these organisms invade the skin tissue, outcompeting the body’s natural flora.
At Grazia Skin, Hair & Laser Clinic, we observe that fungal infections are among the most common dermatological concerns, often exacerbated by humidity, sweat, and improper hygiene. Unlike bacterial infections, fungal issues can be incredibly stubborn, requiring a disciplined approach to treatment to prevent recurrence.
2. Common Types of Fungal Infections
Fungal infections are generally categorized by the area of the body they affect.
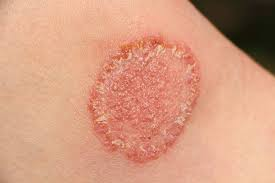
A. Tinea Corporis (Ringworm)
Contrary to its name, this is not caused by a worm. It presents as a red, circular rash with clearer skin in the middle. It can appear anywhere on the body.
B. Tinea Pedis (Athlete’s Foot)
This affects the damp areas between the toes and the soles of the feet. It is highly contagious and often spread in communal showers or gyms.
C. Tinea Capitis (Scalp Ringworm)
Primarily affecting children, this leads to scaly patches on the scalp and can result in temporary hair loss (alopecia).
D. Onychomycosis (Nail Fungus)
A persistent infection that causes nails to become thick, brittle, and discolored (yellow or brown). It is notoriously difficult to treat with over-the-counter creams alone.
E. Candidiasis (Yeast Infection)
Caused by Candida albicans, this thrives in warm, moist skin folds (underarms, under breasts, or the groin). It appears as bright red, itchy patches.
3. Recognizing the Symptoms
Identifying a fungal infection early is key to preventing its spread. While symptoms vary based on the type, look for these “Red Flags”:
- Textural Changes: Scaling, peeling, or crusting of the skin.
- Visual Cues: Redness, circular patterns, or “satellite” lesions (small red spots near the main rash).
- Sensory Irritation: Intense itching (pruritus), stinging, or a burning sensation.
- Odor: A musty or unpleasant smell, particularly in the feet or skin folds.
- Fluid: In severe cases, blistering or “weeping” of the skin may occur.
4. Root Causes and Risk Factors
Fungi thrive in specific conditions. Understanding these can help in prevention:
- Environmental Factors: High humidity and heat (common in tropical climates) promote fungal growth.
- Compromised Barrier: Tiny cuts or abrasions in the skin allow fungi to enter the deeper layers.
- Suppressed Immunity: Conditions like diabetes or the use of immunosuppressants/antibiotics can disrupt the body’s balance.
- Poor Hygiene: Re-wearing sweaty clothes or failing to dry skin folds thoroughly after bathing.
- Direct Contact: Sharing personal items like towels, razors, or combs with an infected person.
5. Clinical Treatment Protocols
At a specialized clinic like Grazia, treatment is tiered based on the severity of the infection.
I. Topical Antifungals
For mild to moderate cases, creams, gels, or sprays containing Clotrimazole, Terbinafine, or Ketoconazole are prescribed. These work by inhibiting the synthesis of ergosterol, a vital component of the fungal cell membrane.
II. Oral Medications
If the infection is widespread or affects the nails/scalp, oral antifungals (Fluconazole or Itraconazole) are necessary. These must be taken under strict medical supervision due to potential effects on liver enzymes.
III. Laser Therapy (Advanced Care)
For stubborn nail fungus (Onychomycosis), Grazia Clinic utilizes Laser Treatment. The laser energy penetrates the nail plate to kill the fungus at the source without damaging the surrounding tissue.
IV. Medicated Washes
Antifungal shampoos (containing Selenium Sulfide or Zinc Pyrithione) are essential for treating scalp infections and preventing the spread of spores.
6. Aftercare and Prevention: The “Dry” Philosophy
The most frustrating aspect of fungal infections is their tendency to return. To stay clear, follow these aftercare rules:
- The Rule of Dryness: Always pat skin dry—never rub. Use a hair dryer on a “cool” setting for hard-to-reach areas like between the toes.
- Fabric Choice: Wear breathable, natural fibers like cotton or linen. Avoid tight synthetic gym wear for long periods.
- Laundry Hygiene: Wash infected clothes, towels, and bedsheets in hot water ($60^\circ\text{C}$ or higher) to kill fungal spores.
- Footwear Rotation: Never wear the same pair of shoes two days in a row; give them 24 hours to air out.
- Don’t Stop Early: Continue applying topical medication for at least one week after the rash has disappeared to ensure the “hidden” fungus is eradicated.
7. Conclusion
Fungal infections are more than just a cosmetic nuisance; they are a sign of an imbalance that requires clinical attention. Through a combination of medical-grade topicals, advanced laser technology, and rigorous lifestyle adjustments, achieving fungus-free skin is possible.
Expert Tip: If you notice a rash that is spreading or not responding to basic hygiene, consult a dermatologist immediately. Self-medicating with steroid creams can often make fungal infections worse by “masking” the symptoms while the fungus grows deeper.
For a personalized skin assessment and advanced fungal treatments, visit us at Grazia Skin, Hair & Laser Clinic.

